Spoiler: Osteoarthritis is the Knee Pain Bogeyman. Let me explain…
The first thing I would like to make clear to any reader that has been diagnosed with osteoarthritis as a cause of their knee pain, is that the pain you feel is absolutely real, in many cases it can be severe, causes an awful lot of disability and most importantly, it deserves an explanation.
It is my strong belief that osteoarthritis is one of the most over-diagnosed, and mis-understood conditions that I see. A simple diagnosis of osteoarthritis can change someone’s life, and not for the better.
So let’s put osteoarthritis in the dock, charged with meaninglessness and creating undue fear, and partake in a bit of cross-examination.
The Word Osteoarthritis is Meaningless
Let’s start this investigation with some definitions.
We’re are looking at the most common form of arthritis; Osteoarthritis. “Osteo” means related to bones. “Arthro” means related to joints and “itis” means inflammation.
So the term literally means bony / joint inflammation. Now the problem I have with this word is two-fold:
- Bone/joint inflammation is more of an observation than a meaningful diagnosis. It doesn’t tell us anything about WHY the person is in pain.
- It creates fear. The word osteoarthritis is synonymous with getting older, wearing out, crumbling away, disability, decreasing mobility and progressing e.g. it only gets worse.
The mainstream information on osteoarthritis is outdated, fearful and needs to change.
So let’s move on from the word itself and start looking at what the current consensus is about osteoarthritis. Let’s start where many of our clients do, in asking wise old Doctor Google.
What does Dr Google have to say about all of this?
I searched for the term: What is osteoarthritis? I immediately got a Google definition:
- “a disease causing painful inflammation and stiffness of the joints”
A disease?! That sounds a bit strong…
It makes it sound like arthritis is like some bacteria or cancer eating away at my joints. And hang on a minute… osteoarthritis ’causes’ painful inflammation and stiffness of the joints?
Let me just go back to that word again; Osteoarthritis = bone / joint inflammation.
So you’re saying, bone / joint inflammation ’causes’ joint inflammation? That doesn’t sound like the most plausible explanation I’ve heard.
Let me put one thing to bed at this moment in time. Knee pain and inflammation are outputs. They are a reaction of the brain to a credible threat to your bodily tissues. They are symptoms of a condition, not the cause.
Ok. So what does Google know anyway? The NHS will know better, they treat the condition all the time. Let’s see what they’ve got to say:
- “Osteoarthritis is a common condition that causes pain and inflammation in a joint”
There’s that word again: ’causes’! How can joint inflammation cause joint inflammation. Lets read on:
- “Osteoarthritis initially affects the smooth cartilage of the joint, the cartilage between the bones gradually erodes, causing bones in the joints to rub together”
What! Where do they get this stuff from?
Come on Arthritis research UK, I trust that they will surely have the answer. Nope! were back to the cartilage again:
- “The main problem is damage to the cartilage that lines the bones”.
A couple of important points to note here:
- Articular cartilage is aneural and avascular, which basically means it cannot be involved in the pain response because there are no nerve endings there.
- I agree that bones rubbing together sounds horrible, but do bones rubbing together cause the problem?
Ok, if all of these respectable organisations are saying that joint degeneration, cartilage damage and bone rubbing on bone is the issue, let’s see how well that argument stacks up in the literature.
Figure 1 below is from Adam Meakins’ blog and shows the results of a study by Guermazi et al.
This group looked at the knees of participants that did NOT have knee osteoarthritis. So basically asking the question: if osteoarthritic knees are caused by abnormalities of the cartilage, what do good knees look like.
72 participants showed signs of osteophytes (extra lips of bone) and had absolutely NO pain, 25 had meniscal lesions and absolutely NO knee pain.
Let’s look at the good old cartilage, 68 participants showed signs of cartilage damage but absolutely NO Knee Pain!
If damage to the cartilage was the cause of knee osteoarthritis, these findings would show that everyone that had damage to their cartilage would have knee pain, and that’s just not true. There is much more to this condition than what you see on a scan.

Figure 1: Prevalence of abnormalities detected by MRI in adults without osteoarthritis
The thing that I want you to take away from this graph, is that it is clear, that our bodies change as we get older, but how our body looks, does not correlate well with pain.
So would it not be better to change the terminology we use and stop scaring the life out of patients. Let’s ditch these fear inducing diagnoses and explanations and just use the term knee pain, and set about working out why the individual has knee pain.
This is 2015!, come on, surely we know that degeneration, and changes seen on imaging, are not well linked to knee pain.
Understanding Osteoarthritis Knee Pain
To understand joint pain, especially in runners, you have to understand both pain itself, and the law of adaptation:
Pain
We know so much more about pain in 2015, we’re still a long way from knowing the full picture, but we are certainly far enough down the road to leave the current explanation of osteoarthritis in the ditch.
Joint pain is complex, multi-factorial, individual, and it changes over time. But just because it’s complex, doesn’t mean it’s complicated, or should be seen as such.
It just needs to be understood. Figure 2 below is a list, not exhaustive, of some of the things that can influence pain, it will serve the purpose of illustrating that pain is multi-factorial and can be influenced by many things.
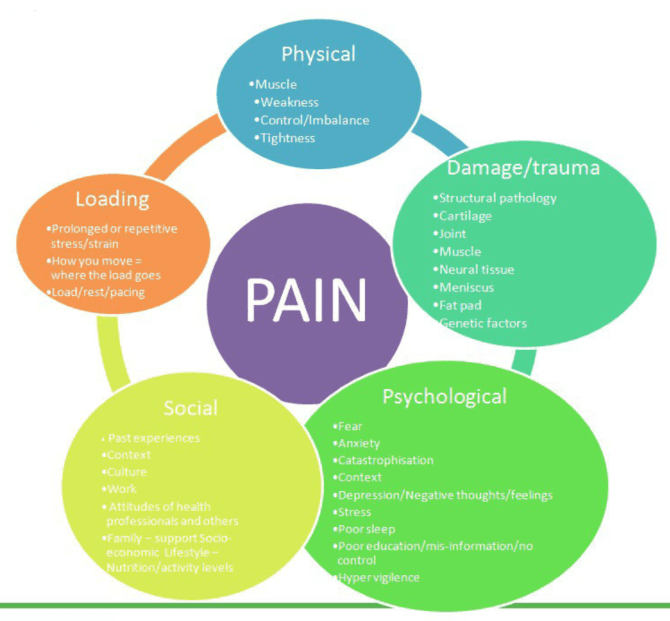
Figure 2: Multi-factorial nature of knee pain
I think that most people have a good understanding of the ‘physical’ and ‘damage / trauma’ factors, and can easily associate them with pain.
But I don’t think the general public, and more importantly, many health professionals, have a good grasp of the psychological and social aspects of pain.
The other thing to bear in mind, is, that on first glance, that list of things looks pretty overwhelming, but no-one will have all of those things going on. The skill of diagnosis is to evaluate which of those things are playing a part in this individuals pain.
Intuitively, to get a good outcome you have to address every element that is effecting that pain experience.
So to return to one of our original questions; what causes Osteoarthritis Knee Pain? I would say the answer is: it depends on the individual.
It is a complex picture, but can be worked out with the right tools. Go back to the diagram in figure 2.
It could be all of those things and more, but it’s likely to be a few. There is an obsession in medicine on trying to zoom further and further into the joint itself, looking for answers, when we should be zooming right out…goodbye joint, hello person…put the scan / x-ray to one side for a moment and engage.
Tell me what you’ve been up to…
What’s going on in your life…?
How much load have you put through that knee recently…?
Are you worried about anything…?
Let’s watch you move…
Stop worrying solely about cartilage, inflammation, degeneration etc.
Red flags aside (red flags are serious pathologies) your knee pain is caused by what you have been doing, how you have been doing it, plus or minus psychosocial factors, not this mythical entity osteoarthritis!
Osteoarthritis is not something you contract, it doesn’t eat away at your joints, it’s just a posh word to describe knee pain!
But wait, I hear you cry! I’m a runner, we are a special group. We spend hours pounding the pavement and putting more stress through our joints, than the average person in the street. This has to have an effect, no?
Yes, it does. A positive one:
Check out this snippet from Cymet & Sinkoc (2006) entitled Does long-distance running cause Osteoarthritis?
“Although there are not currently enough data to give clear recommendations to long distance runners, it appears that long-distance running does not increase the risk of osteoarthritis of the knees and hips for healthy people who have no other contraindications for this kind of physical activity. Long distance running might even have a protective effect against joint degeneration”
And there’s more: Chakravarty et al (2008) took 45 long distance runners and 53 controls (mean age of 58) and took serial X-rays from 1984 to 2002. They found that runners did NOT have more prevalent Osteoarthritis on radiographs compared to control subjects.
Adaptation
In runners with joint pain, I cannot emphasis enough, the importance of understanding loading and adaptation.
So what do I mean by adaptation:
It’s important to understand, that your body is not like an old pair of slippers, that wears out over time, or the more you use it. It is an intelligent, living organism, constantly adapting to the environment. This means that:
- If you don’t put any stress through a joint, it will de-condition. So, if you then decide to use this de-conditioned joint, it will not take much to overload it, and injury / sensitisation can occur.
- If you put too much stress through a joint, it will overload it, and injury / sensitisation will occur.
- If you put an adequate amount of stress through a joint, and then give it an adequate amount of recovery, and you do this consistently – that joint will strengthen! It will adapt and be able to cope with the demands you are placing on it.
The below graph is taken from Blaise Dubois of the Running Clinic, who illustrates the adaptation process nicely here.

The premise itself is very simple, but the reality is far from straightforward. Knowing how much stress, is the right amount of stress, to put us in the ‘adaptation zone’, is very difficult.
The ‘adaptation zone’ will be different from person to person, and just to make it even harder, will change from day to day (probably from hour to hour).
Is the exercise stress needed to hit the ‘adaptation zone’ the same following a day of intense training, compared to an easy day?
Is it the same following a week of stress and no sleep?
What if my athlete turns up and says they’ve had an argument with their boss and haven’t slept all night worrying about it, should we do the same programme I had planned? or do we adjust?
Unfortunately, I don’t have all the answers, but it illustrates the difficulty in getting it right. Prescribing the right dose of exercise, to get the desired adaptation, is often seen as much an art of coaching, as a science. It takes trial and error, understanding of your body, or understanding your athlete, and understanding all the factors that can change where the ‘adaptation zone’ is.
Having said that, to offer some simple, practical advice, I think the guideline of pain during running, pain after running, or excessive morning stiffness is a really nice, simple marker, to know if you may be pushing things too hard and in danger of injury.
Pay attention to these things in your training programme.
Conclusion & Take Home Points
- I propose we need a change in the way osteoarthritis is viewed and discussed.
- Your pain is real and it deserves an explanation.
- The word Osteoarthritis means bony/joint inflammation.
- Osteoarthritis is more of a description than a meaningful diagnosis.
- Pain and inflammation are symptoms and not causes.
- The proposition that damage to a joints cartilage as the cause of osteoarthritis is at worst refuted by the literature and at best just a very small part of a multi-factorial problem.
- Joint abnormalities are seen in people with no pain and are more prevalent the older we get.
- Diagnoses such as osteoarthritis, spondylosis, spondylitis, wear and tear, degenerative joint disease do not describe the condition well. They can be seen as threatening and, in my opinion, should be discontinued as a way of explaining joint pain.
- Joint pain is multi-factorial, individual and can change over time
- Running does not cause osteoarthritis and is likely very good for your joints.
- Diagnosing the cause of knee joint pain means evaluating all elements of the pain response and working out which ones are at play in this individuals pain state.
- The body will adapt and get stronger if the applied stress is not greater than it’s capacity to adapt. Use this information to pace your training.
So runners… don’t stop running, enjoy every minute of it.
Running is not only good for your joints, but just about every system in your body. But before you going bounding out the door, remember to have knowledge of the multi-factorial nature of pain and have a healthy understanding of the law of adaptation.
Resources such as the NHS website and Arthritis UK: Update your information!
I believe with all my heart that the information placed on your sites is there to help people, but it’s becoming part of the problem and strengthening negative, mis-informed beliefs, that is in turn, creating poorer outcomes for patients, not better. It has to change.
And for those that think I’m just one person saying this, and maybe have cherry-picked a few articles, here’s a snippet from the NICE guidelines on osteoarthritis, published in 2014.
For those of you that don’t know, NICE stands for the National Institute for Health Care Excellence, and provide national guidance and advice on health and social care. What do they have to say on osteoarthritis?
“Osteoarthritis refers to a clinical syndrome of joint pain accompanied by varying degrees of functional limitation and reduced quality of life. It is the most common form of arthritis, and one of the leading causes of pain and disability worldwide. The most commonly affected peripheral joints are the knees, hips and small hand joints. Pain, reduced function and effects on a person’s ability to carry out their day-to-day activities can be important consequences of osteoarthritis. Pain in itself is also a complex biopsychosocial issue, related in part to a person’s expectations and self-efficacy (that is, their belief in their ability to complete tasks and reach goals), and is associated with changes in mood, sleep and coping abilities. There is often a poor link between changes visible on an X-ray and symptoms of osteoarthritis: minimal changes can be associated with a lot of pain, or modest structural changes to joints can occur with minimal accompanying symptoms. Contrary to popular belief, osteoarthritis is not caused by ageing and does not necessarily deteriorate. There are a number of management and treatment options (both pharmacological and non-pharmacological), which this guideline addresses and which represent effective interventions for controlling symptoms and improving function.”
Some key the phrases from this to remember: “complex biopsychosocial issue” “poor link between changes on X-ray” “not caused by ageing” “doesn’t necessarily deteriorate”.
The prosecution rests, your honour.
FREE DOWNLOAD: Runner’s Knee Rehab Resources [PDF]
Exercises in Osteoarthritis Knee Pain
It’s always difficult giving general exercise advice, in a condition that’s so individual. But in order to give you some guidance I would say exercises for knee Osteoarthritis pain should be based on SI factors. SI stands for your severity and irritability.
The severity of your pain can be placed on a simple 10 point scale, 0 = no pain, 10 = excruciating pain.
Intuitively, the higher the number, the more severe your pain. Irritability, basically means, that if your pain is brought on, how long does it take to settle.
If the pain goes immediately, it is of low irritability. If it takes hours or days to settle, it is of high irritability.
The higher your SI factors the gentler, and less stressful, the exercise should be, to begin with. I say to begin with, because if you respect the law of adaptation and understand pain you should be able to progress through to more challenging exercises.
There are no ‘bad’ exercises for knee pain, or any condition for that matter. It’s just about understanding that some exercises are more stressful on the joint, than others, and additional factors such as adding weight, increased repetitions, duration, speed, surface, footwear will also effect the stress going through the joint.
Exercise-wise, it appears that a combination of strengthening, around the knee and hip, along with cardiovascular (CV) exercise works well.
For me, I also like to look at your painful movement as well. So, if you get your pain when you run, then I want to see you run, and see if there are any changes we can make, to make it less stressful for your knees.
In terms of pain when exercising. Ideally I would like the exercises to be pain free. Some discomfort is OK, but my general cut off is nothing over a 3-4/10 on a pain scale and that settles within 24 hrs. If it’s more than that, do not stop, adjust the exercise to make it easier so you fall within the above parameters.
Below are some examples of exercises. This is not an exhaustive list, but may give you an idea of where to start based on your SI factors.
Cardiovascular Exercise
Choose whichever makes you happy and is pain free. Examples include swimming, water aerobics, cycling, cross trainer and walking. Start at a low level of intensity/duration and build from there.
Knee Rehab Exercises





This is a fantastic article! There seems to be a trend in healthcare and certainly the NHS at the moment to provide patients with a diagnosis that merely states the individuals symptoms. As someone that has been diagnosed with medial tibial stress syndrome, I can completely emphasise with this problem. In my experience, giving a patient this sort of diagnosis, when they are already in a vulnerable state due to the pain/injury they are suffering, only serves to increase anxiety and potentially the pain. There is a fine balance between providing enough stress to a joint/bone/muscle to initiate adaption and strengthen it. I always think that knowledge is key, and with the information provided in your article, I feel more confident on finding the right balance, thank you.
Hi Claire,
Thanks for your comments. I agree that the diagnoses we give sometimes are counterproductive to our main goal of helping people. We’re very good in the medical world at coming up with complex, scary sounding words to describe the most harmless of things. Creating fear around an injury is a sure fire way to prolong pain!
A great article and is relevant to my experiences with an ankle diagnosis. At the age of 19 I was diagnosed with secondary osteoarthritis in my right ankle. This restricted my movement somewhat I had an operation where they flushed the joint out and put some cortisone in there. It didn’t really make any difference. Luckily I could play basketball still if I had on heavy ankle supports. Which I wore for the rest of my career, never being pain free.
When I retired from playing Nationally League due to back injury I looked for something to do to keep up my fitness and took up jogging, after some initial stiffness and pain within the joint it began to subside to the point where my ankle was pain free for the first time in over 15 years. Even to the point where I can play local league basketball without my ankle supports.
What do I put this down to well it could well be that there was a strength issue within the ankle joint that was causing an imbalance that the running training built up.
The thing was after my initial operation my consultant said that there was nothing that they could do and just left me to it. This article goes a long way in showing that there could be a factor that is causing your osteoarthritis and maybe it can be improved.
Hi Jon,
That’s a great story. Fantastic example that the human body is a wonderful, adaptive organism. We are much more than a picture (X-ray/scans etc).
Firstly excellent article.
Secondly as part of my work I run knee and hip pain rehabilitation classes where the people referred to me have been diagnosed with osteoarthritis in most cases. What is common amongst them is that they have joint alignment issues that place excessive load on the particular joint(s). With corrective exercises this pain can be significantly reduced and in many cases eliminated. I have what I call rule number one, ‘knee above foot’ there are various techniques used to get clients to achieve this. The important points are that when looking from the front the knee is above the foot and not dropping inwards or less commonly moving outside the line of the foot. If the knee joint is not above the tibia then there is nothing supporting the weight above it except the stressed ligaments, tendons and muscles and cartilage. It’s these stresses that cause the pain. Side on to the client the knee should still be above the foot when stepping up for example. The knee should not be in front of the toes or behind the ankle. My rule number two is a little more flexible but the principle should be applied which is shoulder above knee, the load bearing knee that is. Again the application of this is generally stepping up and down but also in squat and sit to stand. Really it is simple physics. And it is the same principle James looks for with running technique at point of loading the knee is above the foot and the shoulders are above the load bearing knee.
Thanks for highlighting such an important part of rehab. How you move, the shape your body makes i.e biomechanics, can give us an insight into where the load is going. As you rightly state, making changes to the way someone moves, can shift the load from the sensitised tissues and allow desensitisation to occur. It’s an incredibly important part of what I do and can make an instant impact.
Dear Jonathan,
Is it possible to obtain your email in order to contact you. I’m very interested in your approach.
Thank,
F
Hi Francois,
Yes you can email me via [email protected].
Regards
Jonathan
About ten years ago my wife had a bit of knee pain while running. A physio diagnosed osteoarthritis and suggested that my wife long longer run any more than 5 miles. She was only 30 so we decided that the odds of this being correct were small and to take it slowly and build back up. She’s since run countless half marathons, several half Ironman distance triathlons and a marathon, with no knee pain. I get the feeling you’re right about this being over diagnosed!
Well, i’m glad your wife didn’t take that advice! and a brilliant story that highlights the poor understanding of the condition. The scary thing is, most of the rubbish i hear is coming from the medical world! physios, GP’s, Consultants!! what chance have our patients got? As you rightly allude to, OA is diagnosed far too often, based on limited information. There’s also this belief that anything that loads your joint (which running does) must be bad for it? It’s so misinformed – it shows a complete lack of knowledge of the human body and adaptation. And why is running always the bad guy! the amount of people that I have seen that have been told they shouldn’t run because it’s harmful or they’re not built for it etc it’s alarming. Can you imagine if I started that advice for all the other conditions i see –
“Hi Physio, It hurts when i lift my arm”
“Ok, don’t lift your arm anymore – NEXT”
“Hi Physio, it hurts when i look over my right shoulder”
“Well stop looking over your shoulder and the pain will go away – NEXT”
Would make my job a lot easier though 🙂
What an excellent article and one that concurs with my own experience. I have been diagnosed with arthritis of my hips. Last August I was seeing a consultant about a total hip replacement, the pain in one hip getting worse and worse. A prognosis I had been expecting for 20 years or so. This followed a period of some inactivity but also came just before I got a place through the ballot in the London Marathon. Not being content with THR as a solution, I took to the internet and came across a discussion of trigger point therapy by someone who had a similar experience. What a revelation. I am now convinced that my pain was not caused by the worn joint (the x-ray clearly shows this) but by poor muscle condition and “alignment/balance”. I ran over 400 miles in preparation with barely a murmur from my hip. I now have issues with my knees that seem to be from the build up of training miles as the article suggests. The click that I thought was coming from my hip is actually coming from my knee. My first thought was oh no, it is arthritis! Your article makes me think otherwise and that there must be a way to manage the pain in my knees as per my hip. Maybe James’s knee rehab programme. Thanks again.
Hi Tim,
I’m glad you found an active approach to managing your hip pain. I’m sure a similar approach to your knees will also help. James’ knee rehab programme is an excellent place to start. Just make sure you’re gradual with your running mileage and, although some discomfort is ok, try not to run or exercise through pain.
Fantastic article – Really drives into expelling myths associated ‘conventional wisdom’ that is unfortunately perpetuated by various misinforming outlets. There seems to be a great deal of this in the Sciences…
Thank you for your kind words. I totally agree. There is far too much misinformation and myth out there, dressed up as science. I really feel strongly about putting out positive health messages and giving the general public all the information they need to make informed choices about their health. It’s the absolute minimum people deserve.
Great article- already sent the link through to one of my patients!
Got quite excited when I received this article in my inbox. I have just had X-rays on both knees as I have been running for 10 years and have just started to get mild knee swelling in my left knee after long runs (10 miles +). I had surgery 30 years ago for patella dislocation so have a predisposition of osteoarthritic changes at some point. To my disappointment my results revealed moderate osteoarthritis in all compartments of both knees. The good news is that I do not have any pain. I love running but do not know how I should proceed now. Do you have any advice please?
Thanks lots to consider.
Our lectures are very good at steering us away from previously accepted principles of OA but your article brings it all together.
This will help with a practical exam on the horizon.
Thanks
Neal
Physio student
Very thought provoking article. I need to keep experimenting with my adaption zone and continue with the ‘stronger hips for pain free knees’ programme, seems to be working so far.
Thanks for the comment Tom! Best of luck with the programme 🙂
Firstly this was a very interesting article that looked at the issue in a different way. I’m presently in week 4 post operative recovery from a high tibial osteotomy performed due to a diagnosis of osteoarthritis in the medial rear compartment of the left knee. For the last five years I have heavily competed in running events and triathlon up to marathon and Ironman and I know from the consistent loading through the knee it was a contributing factor in the presentation of osteoarthritis but I know it’s not the reason. It’s not something I caught or hereditary in my family it’s purely down a trauma 28yrs ago playing rugby and sustaining a full disclocation, this trauma over a period of years has changed the loading through that leg which eventually caused my leg to become varus on a long leg alignment . The only reason this was picked up was I twisted my knee at the bottom of a hill run and made a significant tear in the meniscus which caused the pain and discomfort, upto that point I was running 3:25 marathons.
I have had an 11mm open wedge osteotomy, medial menisectomy and an actifit medial implant, the team are confident I will return to sport but will just need to adjust amount of impact loading to make sure it lasts as long as possible.
The issue was never osteoarthritis it’s was how the leg was loaded.
Great article, I currently have knee pain on the inner side of my right knee, I have sen a sports physio and an osteopath, both with 2 different conclusions, one says it’s a muscle weakness on my right side and the other says possible meniscal tear, ones says keep running and the other says don’t run? I honestly don’t know where I am. I have no pain when running it feels fine, but have some pain on the inner side of my knee after running, I also suffer from chronic pelvic pain syndrome related to my prostate, not sure if this can be related
, but only had this problem after 2 years of running, so I doubt it can be that, I am still awaiting a NHS appointment and hopefully a scan to confirm what the problem is, my anxiety has risen since this injury and I noticed you mentioned this. Question is do I continue running? Feeling lost.
Hi, your article makes interesting reading. I developed hip pain a few months ago whilst running. It feels like it’s coming right from the joint. I thought I would rest it and now it’s so much worse due to inactivity. I have been caught in the trap of going down the painkiller route (that made me sick) and I have just had an xray for which I’m awaiting results ( they are querying osteoarthritis). It’s so difficult to know what to do! In my head I think I should exercise it and I so miss my running. Your article has given me hope. My plan is to start off gently again and not only run but spend time doing some yoga/Pilates to help build up the muscle.
Hi amazing article I have been suffering with my knees and seem to be worse if I drink diet coke? The inflammation thing is very interesting – any connection between diet and inflammation? X
Really enjoyed reading this and it was refreshing to know that I am doing things right! I also start by asking my clients what is happening in their lives at the moment, and what were they up to in their lives when they first noticed their ‘knee pain’. I always tell clients that the human body does not fall apart for no reason and the causation is often over looked as they spend too much time and attention focusing on the pain.
I work with many PT’s in the local area and I really think it is important to hammer home that not every session can be the same.You can’t ‘smash it up’ every time you step foot into the gym. The link between the psychogenic aspect of pain and the physical is still overlooked and is something any body worker whether that be a therapist or personal trainer or coach needs to learn more about. People want to be diagnosed and labelled. Pain is fascinating and is something I am interested in learning much more about. Thanks again!
Terry and James, thank you for a very insightful article.
A very stubborn painful big toe as well as a stress fracture in my foot led me to see a podiatrist after several months of pain (Aug-present) his initial diagnosis for the pain in my toe is osteoarthritis, subject to a scan.
If this turns out to be the case, is there anything I can do to get back running pain free? The pain in my toe causes me to run on the outside of my foot, hence the fracture.
I’ve been swimming and cycling and not running but my toe still hurts, especially after walking for a while.
Any ideas?
Dennis
Hi, this is brilliant to read. I had a painful and swollen knee several years ago was xrayed and diagnosed with O/A. I gave up on running because I thought I shouldn’t be, I then decided to google osteoarthritis running and found this ! now running weekly with no pain and its fab to be able to. I am going to do knee strengthening exercises in gym. Swim and cycle. I am human again.
This article and explanations contained within go a long way to explaining my situation. I am 57 and have been told/shown that I have severe OA in both knees and moderate AO both hips. I am a Remote Area (Wilderness) Firefighter backpacking loads of 35+ Kg up hill and down dale. Each year I pass the APT – Remote Area Firefighters are required to pass an annual task based assessment to the arduous level. The Arduous Pack Test requires the candidate to walk a distance of 4.83 km over level ground wearing a 20.4 kg weight vest. The walk must be completed in 45 minutes or less. Last time I ran; several years ago, both my knees blew out and had to be rested for a couple of days. I consulted a physiotherapist who assessed my ability to hop which I could do on left leg only and concluded that I should no loner run, now if I could run again it would make my training program so much easier and more interesting. So how do I get running????????????????????
Great article. I have been diagnosed with an arthritic hip. I continue to run but sometimes it’s quite painful. People keep telling me to give up running but I would also miss the social aspect so chose to ignore this. I would love a set of excercises for the hip to help this problem and keep me running.
Hi, another great article, big fan of the page.
I am going through a bit of an ordeal at the minute myself with links to the above article.
31 year old male triathlete.
Recent and ongoing knee pain (8 months) escalated even after months of rehab for muscle imbalance, quads, hip flexors, glutes etc. Recent MRI scan showed bone marrow edema and stress fracture on left medial tibial plateau. Further complicating factor is bone marrow edema on both femoral heads about 12 months ago which has since completely resolved. Developed knee pain at a time when not running at all (2 months). Doctor saying maybe transient migratory osteoporosis, other doc not so sure – linking current knee injury to me being ‘slightly bow legged’ and could be linked to increased biking load. The only running done in last 11 months was easy 20 mins of 1 min run, 1 min walk (about 4 sessions) before knee pain became too much. Blood tests all normal & awaiing results on bone Dexa scan. Pain not too severe at all with both injuries but increases with activity. My left knee does a lot of crunching when flexed then extended but not painful. No cartilage or other damage noted on MRI.
Don’t really have a specific question as such but your article re knee pain intrigued me & was just wondering if you had an opinion on the above. Been a bit of a nightmare 12 months or so!
Thanks in advance
Mark
Thanks so much for this information. I have been dealing with Osteoarthritis on and off since October and I have visited several docs but they can’t tell me what is causing it. One of my friends told me about RS4supplements.com and PeaPlex is very helpful therefore.