How to Treat ITB Syndrome in Runners

In this article, I'm going to clear up some common misconceptions surrounding ITB syndrome and help you discover the root cause of your knee injury.
Once you know what causes ITB syndrome, you can begin the rehab process and build towards a full return to running.
What is ITB Syndrome?
Iliotibial band (ITB) syndrome is a common running injury which is frequently misunderstood and treated poorly. This is despite how very common ITB syndrome is amongst distance runners.
I'd like to share with you how I treat runners with ITB syndrome from a biomechanical standpoint. Taking this approach will help you successfully treat the underlying cause of your problem.
Iliotibial Band Anatomy
Let us start by refreshing our anatomical understanding of the iliotibial band itself.
The iliotibial band starts around the hip with insertional fibres of both gluteus maximus and tensor fascia lata. Lower down, around the knee region, it inserts into gerdy’s tubercle on the lateral aspect of the tibia, passing over the lateral femoral condyle.
To protect the iliotibial band from the lateral femoral condyle there is either a bursa (fluid filled sac) or a layer of highly innervated fat that lies underneath the distal portion of the band [1].

It is essential to remember that the iliotibial band is nothing more than a longitudinal fibrous reinforcement of the fascia lata and has no control over its own positioning or tone. It cannot contract as a muscle would, and we cannot stretch the IT band.
The IT band attaches to the intramuscular septum of the femur in a variety of places (this is a natural variant of IT band anatomy) via fascial strands which pass through the periosteum (lining of the bone), rather than merely attaching to the surface.
The tension within the IT band will ONLY increase when the origin and/or insertion move further apart and we will discuss how this can occur later on.
I would, therefore, question what one of the most common IT band syndrome treatment techniques employed to tackle ITBS, foam rolling, is physiologically achieving. Attempting to release a non-contractile tissue which has the tensile strength of steel and is anchored firmly to cortical bone, isn't going to work.
Image via @afranklynmiller. Illustrated by Levent Efe
What Causes ITB Syndrome?
I'd argue that ITB syndrome is more related to compression than friction, as was previously believed [1]. In fact, it has commonly been known as ITB friction syndrome - a name we now know as being misleading.
Let me explain...
The pain stimulus within ITB syndrome is usually inflammatory, whereby either the bursa or fat pad is compressed against the lateral femoral condyle. This will occur whenever the IT band is put under more strain by a change of position at either its origin or insertion.
Compression (for example lying on the affected side) can be a factor which exacerbates ITB syndrome symptoms. Similarly, another common pattern is that pain can be more severe first thing in the morning. It will often respond well to oral non-steriodal anti-inflammatory drugs (NSAIDS).
A clinically beneficial option may be to have the region examined under real-time ultrasound scan, which will determine the need for a guided corticosteroid injection, which can provide a positive reduction in symptoms in severely irritable cases.
Cortisone Injections for Runner's Knee? Here's What You Need to Know… <- Learn more about steroid injections for knee pain here
It is here that I will point out that the dreaded foam roller can often exacerbate knee pain symptoms, by further increasing the compression against the lateral femoral condyle.
What Causes IT Band Syndrome?
There are a number of common biomechanical factors that cause ITB syndrome in distance runners, especially when these factors are exacerbated by an increase in running training volume.
These include:
1) Hip Flexor Imbalance
One biomechanical flaw that will cause an increased strain of the iliotibial band is hip flexor imbalance.
Poor iliopsoas function will result in a compensatory firing of tensor fascia lata, which has the ability to assist with hip flexion because of its anatomical lever arm [2, 3]. Over a period of time, the length of the tensor fascia lata will reduce (become hypertonic), which means that the Iliotibial Band origin moves AWAY from the insertion. A secondary consequence is a rise in the anterior hip joint forces and an excessive abduction moment, which is counteracted by an additional compensation within adductor longus.
An underactive Iliopsoas muscle is very common within running athletes who have a tendency to use rectus femoris, one of the quadricep muscles, to generate hip flexion, instead of iliopsoas. This is an extremely common running technique flaw.
Why do some runners overuse rectus femoris? <- Learn what causes this kind of imbablace, and how you can fix the problem...
The hypertonicity of tensor fascia lata can be effectively treated with targeted soft tissue release. In my opinion, this is most effectively performed with a large acupuncture needle, to manipulate the myofascial restriction and release any myofascial trigger points within the muscle. Hands-on soft tissue therapy would also be a good option if you prefer.
For those of you that are fans of the dreaded foam roller, please roll local to the tensor fascia lata (roughly near your pocket on a pair of trousers), but remember that muscles and tendons aren’t amazed by compression either, and that you run the risk of causing gluteus medius tendinopathy as a result [4].
2) Dynamic Knee Valgus
The most commonly seen biomechanical flaw in the running population is dynamic knee valgus, a combination of femoral internal rotation with adduction and tibial internal rotation [5].
This will result in the insertion of the Iliotibial Band moves AWAY from the origin. A high-quality prospective study by Noehren and colleagues [6] linked this pattern to patients with ITB syndrome symptoms.
Dynamic knee valgus can occur as a result of several muscle imbalances but the most common pattern that I see is a weakness/inhibition of gluteus maximus.
Knee Stability Exercises for Runners <- Try these simple exercises which will help you better control knee position
I feel that gluteus maximus is more influential than gluteus medius in this presentation as it is a three-dimensional single joint muscle, the most powerful external rotator of the hip and the superior fibres contribute significantly to hip abduction. Gluteus medius contributes by fixing the pelvis relative to the femur [7].
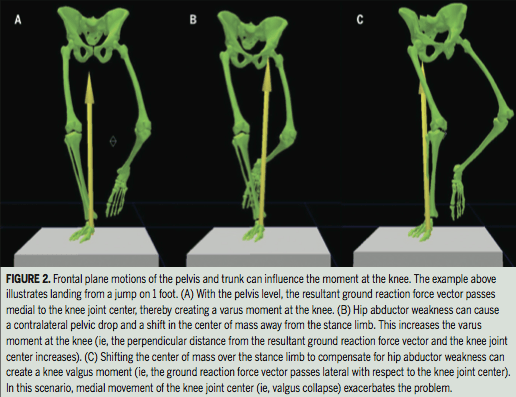
IMAGE © Journal of Orthopaedic & Sports Physical Therapy
3) Contralateral Pelvic Drop / Hip Drop
A highly relevant biomechanical flaw within ITB syndrome is a contralateral pelvic drop, also known as "hip drop".
This occurs in single leg stance, with the pelvis dropping down on the non-stance leg relative to the femur in the sagittal plane.
This will result in a subsequent lift of the pelvis on the stance leg, meaning that the origin of the iliotibial band moves AWAY from the insertion. This occurs as a result of a much more specific pattern of muscle imbalance, whereby gluteus medius on the stance leg, and a combination of quadratus lumborum and external oblique muscles on the non-weight bearing side of the torso, fail to fix the pelvis relative to the femur.
How to Fix Your Hip Drop <- Check out this article for more information about this type of running gait, and how to improve hip stability
This pattern often results in over-activity within the lateral trunk on the stance limb and can be a significant contributing factor in patients with unilateral spinal pain.
How Long Does it Take for ITB Syndrome to Heal?
Given the correct treatment and knee rehabilitation plan, you can expect ITB syndrome to heal in 6-12 weeks. It largely depends on the severity of the case, with some runners able to return to full training much sooner, and others requiring a longer period of rest and rehabilitation.
Understandably, any runner with this knee injury will want to know how long it takes ITB syndrome to heal, but you should be guided by your physiotherapist, as each case is different.
Key Points for IT Band Syndrome Treatment
- The point that I would like all readers to go away with is that it is muscle imbalance, and not a “tight” IT band that causes this common problem and that it is rehabilitation (activation/strengthening) and not compression/stretching that will cure your symptoms.
- Please remember that we are not robots and not all patients will fit into these simple biomechanical boxes.
- People often present with combinations of these movement patterns and certainly dynamic knee valgus can be as a result of many muscle imbalances, which I will happily elaborate on in the discussion section of the blog if the questions arise.
- The challenge for clinicians is to identify them, rehabilitate them and most importantly teach the patient how to transfer what they learn in the gym to their running style.
Here's an example of a simple iliotibial band syndrome rehab routine you can try:
Please do not throw out the baby with the bathwater. There is still a place for (as examples) soft tissue release of the lateral quadriceps, local anti-inflammatory agents for an acute bursa, kinesio taping (a whole other debate!) to reduce pain and facilitate improved movement; but remember that these techniques treat the symptoms and only rehabilitation of the contributing factors will result in long-term improvement.
CLINICAL REFERENCES
[1] Fairclough, J et al (2006). The functional anatomy of the iliotibial band during flexion and extension of the knee: implications for understanding iliotibial band syndrome. J Anat 208, 309-316.
[2] Lewis, C et al (2009). Effect of position and alteration in synergist force contribution on hip forces when performing hip strengthening exercises. Clin Biomech 24 (1), 35-42.
[3] Lewis, C et al (2007). Anterior hip joint force increases with hip extension, decreased gluteal force or decreased iliopsoas force. J Biomech 40 (16) 3725-3731.
[4] Cook, J & Purdam, C (2012). Is compressive load a factor in the development of tendinopathy? Br J Sports Med 46, 163-168.
[5] Distefano, L et al (2009). Gluteal muscle activation during common therapeutic exercises. JOSPT 39 (7), 532-540.
[6] Noehren, B et al (2007). Prospective study of the biomechanical factors associated with iliotibial band syndrome. Clin Biomech 22, 951-956.
[7] Powers, C (2010). The influence of abnormal hip mechanics on knee injury: a biomechanical perspective. JOSPT 40 (2), 42-51.